1 Introduction
People with serious mental illness are overrepresented in the justice system. For example, most county jails in the United States house three times as many people with serious mental illness as would be expected from community-based estimates (1). In this article, we review the complex array of factors that contribute to the problem of the overrepresentation of people with serious mental illness in the justice system and offer suggestions on how an integrated community behavioral health system, including mental health and substance use services, can coordinate efforts across multiple systems to address this problem.
We understand that referring to community mental health and substance use services as a “system” suggests that it is a monolithic entity, when in fact, there is no single community behavioral health system in the United States. Yet this system, no matter how fluid, retains primary responsibility for the care and treatment of people with severe and persistent mental illness. Factors that create variability in the delivery and availability of services in the community behavioral health system include the rising influence of Medicaid and Medicaid managed care, the resulting diminished authority of state and county mental health authorities, the variation among states that did and did not choose to expand Medicaid under the Affordable Care Act, and the efforts to integrate mental health and substance use treatment with the larger health care system (2, 3).
However, despite the varied and evolving nature of community mental health and substance use services, we believe that there are compelling interests—both fiscal and humanitarian—to effectively address the needs of people with serious mental illness who become involved in the criminal justice system, and no system is more familiar with or more equipped to meet the needs of this population than the behavioral health system. This article presents a vision that we hope will help guide the development of new and needed practices and policies to better meet the needs of people with serious mental illness who become involved with the criminal justice system.
This article presents a vision that we hope will help guide the development of new and needed practices and policies to better meet the needs of people with serious mental illness who become involved with the criminal justice system.
2 Unpacking the Overrepresentation of People with Serious Mental Illness in the Justice System
National, state, and local efforts to address the overrepresentation of people with serious mental illness in the justice system have proliferated over the past 20 years. An increasing number of police officers receive training in ways to recognize and safely resolve incidents involving people with serious mental illness through the crisis intervention team (CIT) model (4). In addition, many judges are better equipped to manage mental illness in their courtrooms, and probation and parole departments are developing specialized units (5, 6). More than 500 counties have signed up for the National Stepping Up Initiative to develop reentry programs to reduce the number of people with mental illness in their county jails (7).
Many of these advances were motivated by the criminalization hypothesis, which posits that the overrepresentation of people with serious mental illness in the justice system is the result of deinstitutionalization of psychiatric hospitals, underfunding of community mental health treatment, and tightening of involuntary commitment laws (8, 9). According to the criminalization hypothesis, these policy changes created an overburdened and underfunded community mental health services system. As a result, many people with serious mental illness shifted (or drifted) from psychiatric institutions to the criminal justice system. The criminalization hypothesis as originally conceptualized offered an overly simplistic view that the overrepresentation of people with serious mental illness in the justice system was primarily due to their transinstitutionalization from mental health settings into the justice system. This is why we believe that there is a need to refocus our understanding of and approach to addressing the multiple factors that contribute to justice involvement of this population.
First-Generation Criminal Justice Interventions
The criminalization hypothesis led to the development of “first generation” mental health and criminal justice interventions (10, 11). Although the content and structure of first-generation interventions vary, the central assumption is that access to mental health services is essential because untreated mental illness is believed to be the key driver of justice involvement for people with serious mental illness (10, 11). First-generation interventions for justice-involved people with serious mental illness include programs such as pre- and post-booking diversion programs, mental health courts, specialized probation, forensic assertive community treatment teams, and reentry programs. Although many of these programs are innovative and have shown promise at improving mental health symptomatology, none have been able to achieve a sustained impact on criminal recidivism (12–15). In fact, the service models with the weakest impact on criminal recidivism among justice-involved people with serious mental illness are those most closely aligned with traditional mental health treatment (14), suggesting that factors other than symptoms of mental illness contribute to justice involvement for this population.
Over the years since the criminalization hypothesis was first postulated, factors associated with criminal justice involvement among people with serious mental illness have been identified. For example, research has found that justice-involved people with serious mental illness have especially high rates of co-occurring substance use disorders that complicate their involvement with the justice system (16). People with co-occurring mental illness and substance use disorders recidivate more often and more quickly than do those with serious mental illness only (17–21). Yet even evidence-based approaches, such as integrated dual-diagnosis treatment, have failed to reduce justice involvement of people with serious mental illness (22, 23). This suggests that although integrated treatment of mental and substance use disorders among justice-involved people with serious mental illness is a necessary part of comprehensive treatment, these clinical services alone will not solve the overrepresentation of this population in the justice system.
The focus of first-generation interventions on mental health treatment as the solution to justice involvement among people with serious mental illness overshadowed other emergent research that suggests that most justice involvement of people with serious mental illness is not the direct result of symptomatic mental illness (11, 24–29). A newer perspective, known as the criminogenic risk perspective, identifies a broader set of factors at play in justice involvement for people with and without serious mental illness. This perspective is derived from the risk-need-responsivity model, which identifies eight risk factors with the strongest empirical connection to criminal recidivism. These individual-level, psychological criminogenic risk factors include history of antisocial behavior, antisocial personality pattern, antisocial cognition, and antisocial associates—called the “big 4” because they have the strongest association with continued justice involvement (30)—and also substance abuse, family or marital conflict, low educational attainment and unemployment, and lack of appropriate leisure activities, which have a moderate association with recidivism (30).
Recent research has lent support to the criminogenic risk perspective by finding that criminogenic risk factors mediate the risk of recidivism among people with serious mental illness. A growing body of research suggests that justice-involved individuals with serious mental illness may manifest the same criminogenic risk factors as those in the criminal justice system without serious mental illness but at greater rates (14, 25–27). Taken together, research on co-occurring substance use and the criminogenic risk perspective illustrate another layer of complexity in the treatment needs of justice-involved people with serious mental illness. However, criminogenic needs are not a focus of treatment in most existing mental health services, which is a situation that must be corrected.
The Four-Quadrant Model
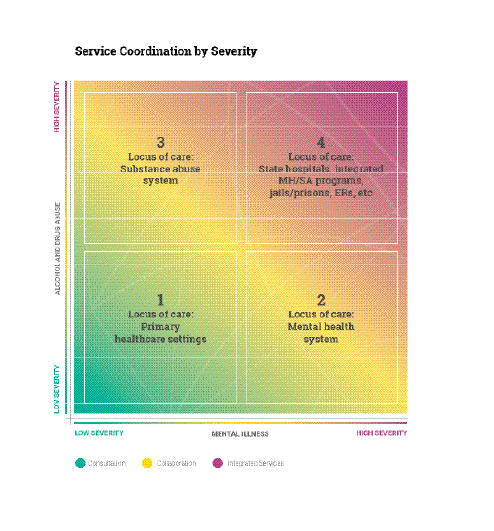
The four-quadrant model provides a framework to guide these integration efforts. This service planning tool conceptualizes the complexity of needs in multiple areas (e.g., mental health and substance use) by considering severity of need (53). Each quadrant depicts possible classification and service responses for clients on the basis of the level of need they manifest for each disorder. For example, people with low mental health and low substance use needs (quadrant I) have different treatment and service needs compared with people with high mental health needs but low substance use needs (quadrant II), and these individuals differ from people with high mental health needs and high substance use needs (quadrant IV).
The complexity of needs of this vulnerable population is why we are focused on making a single system—what we are calling the integrated community behavioral health system—the focal point for services for justice-involved people with serious mental illness. The clinical mental health needs and the substance use needs of justice-involved people with serious mental illness are critical targets of intervention, and providing these services in an integrated and seamless fashion has proved challenging. Further integrating services to address all the treatment needs of justice-involved people with serious mental illness, including criminogenic needs, while also working to develop linkage strategies that facilitate timely access to other essential social services is a big goal. But an even greater challenge is to leave these responsibilities to the criminal justice system, because personnel in that system lack clinical expertise in the treatment of serious mental illnesses, an existing treatment platform on which to build, and a publicly legislated mandate that focuses specifically on the treatment needs of people with serious mental illness.
Therefore, if the community behavioral health system does not step up and accept the challenges associated with expanding its service continuum to address the complex treatment needs and the level of services coordination that justice-involved people with serious mental illness require, this substantial, and very vulnerable population, will be left behind.
We understand the high aspirational bar we are setting for what, in many communities, is a fragmented, often incoherent, system. As noted above, the planning role of state mental health authorities has been diminished, and the funding role has been subsumed through the state Medicaid agencies and the state’s contracted managed care companies (2). Because of these challenges, some advocate for alternative approaches to the vision we describe here. However, given that states have a responsibility to ensure that there is an accountable system for the care and treatment for people with severe and persistent mental illness, whether it is under the direction of the state mental health authority or state Medicaid authority or through careful contracts with managed care companies, there remains a strong interest in reducing overall costs, increasing community safety, and addressing community wellness. As we embark as a field on the development of interventions for justice-involved people with serious mental illness, we believe the time is ripe to develop a new, comprehensive vision of what must happen to effectively address the overrepresentation of this population in the criminal justice system. Opportunities exist for criminal justice and community behavioral health system stakeholders to strategically coordinate and advocate for the mental health and substance use services and the justice and social policy reforms needed to attain the service expansion described above. We explore these opportunities in the next section.
3 The Sequential Intercept Model: A Guiding Framework
To address the overrepresentation of people with serious mental illness in the justice system, the range of services available to meet the complex service needs of this population must be expanded and integrated. We propose that the behavioral health system serve as the central point of contact for providing an integrated array of services for this population. For this approach to be successful, we need a “second generation” of services that prevents or reduces further justice involvement by providing a broader array of treatment services that meet the complex clinical and criminogenic needs of people with serious mental illness (10, 11, 54). We also must intensify efforts to coordinate with other social services to address basic needs (e.g., income assistance, vocational assistance, and housing) in a streamlined and personalized manner. This is a relatively new concept within a field that has long been devoted to the criminalization hypothesis and to first-generation services to engage people with clinical mental health services.
For this approach to be successful, we need a “second generation” of services that prevents or reduces further justice involvement by providing a broader array of treatment services that meet the complex clinical and criminogenic needs of people with serious mental illness.
The sequential intercept model may help achieve this vision. It identifies opportunities for stakeholders from the community behavioral health system and criminal justice system to work together to intervene, diverting people from the justice system to the community behavioral health system. The sequential intercept model provides a conceptual framework to spur the development of a range of interventions designed to prevent justice involvement altogether, ideally by way of an effective, accessible, and criminologically informed mental health treatment system (55–57).
The sequential intercept model proposes five points of contact in the criminal justice system at which a person with mental illness can be “intercepted.” These points include the following:
INTERCEPT 1
interactions with law enforcement and the crisis response system
INTERCEPT 2
initial detention and initial hearings
INTERCEPT 3
jail and courts after initial hearings
INTERCEPT 4
reentry from jail, prison, or a forensic hospital
INTERCEPT 5
community corrections and community support
Originally in this model, the community mental health system was described as the “ultimate intercept,” where people with serious mental illness at risk of justice involvement or who may have other conditions putting them at risk of such involvement, such as trauma, social disadvantages, or substance dependence, could be identified and an integrated treatment or intervention plan could be enacted or coordinated with the appropriate service system (55). Thus the ultimate intercept refers to a treatment and service system that is responsive to the diverse, and at times intricately intertwined, needs of people with severe and persistent mental illnesses — ideally, before they ever become involved in the criminal justice system.
Recently Policy Research Associates, which operates the Substance Abuse and Mental Health Services Administration’s (SAMHSA’s) GAINS Center, introduced “intercept 0” within the sequential intercept model and defined it as encompassing “the early intervention points for people with mental and substance use disorders before they are placed under arrest by law enforcement” (58). Whereas intercept 1 represents a collaborative effort between law enforcement and the behavioral health community to avoid arrest when possible, the concept of intercept 0 recognizes the need for a full crisis response continuum and expands the partnership to broader mental health and law enforcement collaborations (58, 59). The discussion around intercept 0 has effectively mobilized advocacy to expand crisis services, as evidenced by the inclusion in the fiscal year 2020 SAMHSA budget passed by the U.S. House of Representatives of a 5% set-aside in block grant funds to the states to enhance crisis services (60).
Although we fully endorse intercept 0, we believe that it is best conceptualized as a renaming, and perhaps reframing, of what was called the ultimate intercept in the original description of the model. Although crisis services are an important piece of a comprehensive mental health system, they are only one element of the ultimate intercept as originally conceptualized, which also identified the need for evidence-based interventions, including community support services, medications, and vocational and housing services (55). The vision that we are presenting here is for an integrated behavioral health system to serve as the ultimate intercept, as originally envisioned, which we now call intercept 0, to include accessible, effective, and criminologically informed services for people with serious mental illness to help them avoid entering the justice system altogether (55, 57, 61).
4 The Behavioral Health System as Intercept 0
For the integrated community behavioral health system to operate as an effective intercept 0, the system must both widen and deepen its array of services. To do so, it will need to master integration at multiple levels. Mental health, substance use, primary medical, criminogenic, and social needs all must be addressed in a coordinated and timely manner to achieve the desired goals of improved health, prevention of institutionalization (hospitalization and incarceration), and overall recovery.
Incorporating multiple layers of integration into the operation of any one system is challenging, but this type of integration is an essential effort aimed at reducing the overrepresentation of people with serious mental illness in the justice system, and we believe it can be done. Because of its focus on prevention, early intervention, and recovery, the community behavioral health system is well poised to lead coordinated efforts to address the multiple needs of people with serious mental illness who are in the justice system. An integrated behavioral health system can focus on the provision of trauma-informed care to reduce the risk of traumatization as people with serious mental illness become involved (or reinvolved) with the justice system. Prevention efforts around substance use and efforts to intervene earlier in the course of serious mental illness have proven to be effective models of lessening the trajectory and harmful impact of illness (62).
Furthermore, integrated approaches have worked in the past. Historically, community mental health services, substance use services, and overall health care were provided in largely separate systems. To better address the needs of individuals with serious mental illness, there have been considerable efforts to integrate mental health treatment with treatment for co-occurring substance use disorders through integrated dual-diagnosis treatment (63). More recently, there have been major efforts to further integrate behavioral health care with overall primary health care (64, 65), including the current eight-state initiative establishing certified community behavioral health clinics (66).
There is an increasing awareness of the need to address criminogenic needs of people with serious mental illness to prevent justice involvement. Interventions based in cognitive-behavioral therapy that engage a social learning approach to target specific criminogenic needs (e.g., antisocial behavior or attitudes) have been effective in reducing criminal offending (30), and evidence is emerging that these approaches can be effective for justice-involved people with serious mental illness (67). Osher and colleagues (51) developed a shared framework to integrate approaches to address multiple needs that builds on efforts to classify and treat mental illness and substance use disorders (e.g., the four-quadrant model) by adding the dimension of criminogenic risk. In this framework, individuals may be assessed on the basis of high or low levels of criminogenic need and clinical mental health or substance use treatment needs, and if a broader array of clinical services is available, appropriate service engagement can be arranged to meet these individual needs. There is also recent acknowledgment of the importance of earlier intervention in the trajectory of justice involvement by recognizing both individual factors and social conditions that contribute to criminality and justice involvement (33, 68).
For the integrated community behavioral health system to operate as an effective intercept 0, the system must both widen and deepen its array of services.
The community behavioral health system is also well positioned to address the structural risk factors that drive justice involvement of people with serious mental illness (e.g., poverty, homelessness, and unemployment), either directly or through the coordination of services. There is evidence that suggests that addressing these social determinants of health within the purview of the community behavioral health system can lead to successful outcomes. For instance, supported employment and Housing First initiatives have been shown to effectively increase treatment engagement among people with serious mental illness and also help them gain independent housing or competitive employment and reduce criminal reoffending (69–71).
Our vision is also consistent with current directions and priorities at the federal level. In 2017, the Interdepartmental Serious Mental Illness Coordinating Committee, a partnership among U.S. federal agencies to enhance coordination to improve service access and delivery of care for people with serious mental illness, developed priorities for increasing community partner engagement to address social determinants of health, improve service coordination, and create effective jail diversion opportunities (72).
5 Implications for Policy and Practice
Strange as it may seem, having the behavioral health system take the lead in addressing the overrepresentation problem is a significant change in many communities. Justice system leaders assert that they have been placed in the position of taking on the responsibility of justice-involved people with serious mental illness (73). Many of the newer solutions to the problems confronting this population have been led by sheriffs, judges, and other criminal justice system leaders (74).
Although mental and substance use disorders and criminogenic needs all need to be addressed, efforts to make the behavioral health system the focal point for the provision of this care will likely encounter resistance. The community behavioral health system may not want to take on this challenge, the criminal justice system may not want to give up control, and social service agencies may not be prepared for the degree of collaboration needed. Within community mental health systems, justice-involved individuals with serious mental illness are perceived to be qualitatively different from other individuals with serious mental illness. As with earlier resistance to integrate care for co-occurring substance use disorders with care for mental illness, community behavioral health system stakeholders should recognize that justice involvement in the population served is common and not a rare exception. Studies have reported a range from 25% to as high as 71% of people with serious mental illness in community samples who have a history of justice involvement (75–78). Community behavioral health agencies and social service agencies will need to make a commitment to integrating approaches and coordinating efforts to reduce the siloed organization of services. They must also be prepared to accept that justice-involved individuals should not be additionally stigmatized but should be welcomed as an appropriate, and substantial, population to be served (79). Research is needed to improve models of care that can deliver treatments as seamlessly as possible to meet the multiple needs of clients.
Funders of justice and mental health collaborative initiatives may need to rethink funding structures and priorities and ensure that treatment interventions and supports enhance an integrated behavioral health system rather than take place in the justice system. In most parts of the United States, the stark reality is that the publicly funded service system is not adequately supported to take on its daunting tasks. Current efforts to integrate mental health and substance use services within overall health care may run counter to our call for developing specialized service delivery approaches to meet complex medical and social needs of individuals with serious mental illness and justice involvement. We need innovative approaches to funding the behavioral health system that expand service capacity—initiatives such as the certified community behavioral health clinics currently being piloted. These resources may expand further under the proposed Excellence in Community Mental Health and Addiction Treatment Expansion Act.
We also need innovation and adaptability among state and mental health authority leadership. Arizona, for example, has essentially merged its state Medicaid and behavioral health agencies into a single entity and has worked with managed care plans to develop specialized programs for persons with serious mental illness.
We also need innovation and adaptability among state and mental health authority leadership. Arizona, for example, has essentially merged its state Medicaid and behavioral health agencies into a single entity and has worked with managed care plans to develop specialized programs for persons with serious mental illness (80, 81). Ohio may serve as another example of state leadership that has recognized the need for such vision. The state recently created RecoveryOhio, a plan to improve prevention, treatment, and recovery support efforts. Initially focused on the opioid epidemic, RecoveryOhio quickly expanded to include a broader focus on the mental health and substance use system and now emphasizes the need to address the problem of people with serious mental illness in the justice system. Directors of key state agencies work together with the RecoveryOhio director, who reports directly to the governor. Other states may find a model such as this conducive to effecting change to address a problem that they all face.
National initiatives have emerged to improve system responses to justice-involved people with serious mental illness. The Justice Reinvestment Initiatives supported by the Bureau of Justice Assistance, with technical assistance from the Council of State Governments, and the Safety and Justice Challenge, supported by the MacArthur Foundation, are significant efforts to address unnecessary incarceration. The National Partnership for Pre-Trial Justice, supported by Arnold Ventures, has multiple national partners considering best practices in pretrial detention. And the National Stepping Up Initiative provides a framework for local community stakeholders to collaborate across systems to address the problem.
Ultimately, critics and scholars of the problem of the overrepresentation of people with serious mental illness in the criminal justice system need to change the narrative. Instead of blaming overrepresentation on a failed mental health system or lack of inpatient beds, the complexity of the problem and the need for complex solutions must be acknowledged. In many ways, the community behavioral health system is doing the best it can with the resources it has. New initiatives such as the ones described here require increases in funding for community mental health and substance use services; the competency of these systems in integrating treatment of mental illness, co-occurring substance use, general medical conditions, and criminogenic factors must be enhanced, and new integrated treatments need to be developed and studied. In addition, social determinants of health, such as stable housing, employment, and education, need to be integrated, or addressed in coordination, with treatment. Larger social policies that have driven mass incarceration also need to be acknowledged as disproportionately affecting people with serious mental illness but with a recognition that the behavioral health system cannot fix these issues on its own.
Although an array of stakeholders across the behavioral health, justice, and social services systems can become strong advocates for policy change, they (we) must be joined by the public and policy makers alike. We know that broad advocacy works. Recent successes in states that have expanded Medicaid and the passage of the parity laws show that social policy can improve access to critically needed mental health services. The advocacy we need now could include a push for policy reforms and restructured financing models to increase access to integrated behavioral health services.
6 Conclusion
The overrepresentation of people with serious mental illness in the justice system is a complex issue that requires systematic change and collaborative problem solving. We believe that an integrated community-based behavioral health system (i.e., intercept 0) is ideally situated to address the complex needs of this population and prevent criminal justice involvement. If adequately supported, this system could provide accessible, effective, and criminologically informed services to address the clinical, criminogenic, and social support services needs of people with serious mental illness who are involved in the justice system. The goal is to identify people who would be best served in community settings and expand the continuum of services available within the behavioral health system to meet people where they live, work, and receive services. The role of the justice system will move toward collaboration and away from the need to build a parallel treatment system to address the treatment needs of justice-involved people with serious mental illness. We believe that this approach can improve individual and systems outcomes by preventing justice involvement, reducing service redundancy, and improving health and quality of life of people who are living in the community. All of society needs to take on the larger social issues that disproportionately affect people with serious mental illness.





Social Factors That Exacerbate Justice Involvement
In addition to the mental health, substance use, and criminogenic treatment needs described above, the multitude of social problems facing many people with serious mental illness also increases their risk of justice involvement (31). Social problems of poverty, homelessness, unemployment, and low educational attainment accompany serious mental illness (11, 31, 32). An increasing number of researchers and advocates point to poverty as a key driver of justice involvement for people with and without serious mental illness (11, 31, 33). Many people with serious mental illness live in environments and communities where crime, violence, ambient substance use, and social disorganization are endemic, which can increase justice involvement (31, 32, 34–36). Living in neighborhoods with disadvantaged conditions is stressful, which may contribute to poor health outcomes and activate justice involvement for some people with serious mental illness (11, 37). Therefore, interventions attempting to reduce criminal justice involvement in this population must also address the social and economic factors that contribute to poverty and other social problems.
Social policies that have contributed to mass incarceration for the general population have also affected the number of people with serious mental illness in the justice system. Criminal justice policies, such as the war on drugs, and “tough on crime” policies, such as determinant sentencing and “3 strikes” rules, resulted in a marked increase in populations of jails and prisons for the U.S. general population in the 1980s and 1990s (38–40). These policies have been implemented at a national level within a culture of de facto racism in the post-Civil Rights era in the United States, where people of color are subject to unequal protection of the law and increased surveillance, leading to an overrepresentation of people of color, especially black and Latinx people, at every stage within the criminal justice system (40–42). There is evidence that these disparities extend to people with serious mental illness, because some research has found differential exposure to and experiences within the criminal justice system for people from racial and ethnic minority groups who have mental illness and substance abuse use problems (43–45).
Incarceration rates of people with serious mental illness increased along with rates for the general population during this period of mass incarceration, and studies have shown that arrest rates of people with serious mental illness are comparable to rates in community samples (31, 38, 46–49). However, the sequelae of justice involvement are much worse for people with serious mental illness, compared with the general population, because once they become involved in the criminal justice system, they are more likely to become entrenched (17, 49). They remain incarcerated for longer periods for the same charges, are more likely to be viewed as noncompliant, and have more difficulties with correctional or jail staff and other inmates while incarcerated (50, 51). Furthermore, they are more likely to be victimized while incarcerated, compared with the general population (52), contributing to increased trauma and the psychological toll of incarceration.
People with serious mental illness have complex lives that are not defined by their mental illness alone. As with people in the community generally, their reasons for involvement in the justice system are complex and driven by individual-level clinical, criminogenic, and social service needs, and they are also situated within social and political contexts that contribute to their overrepresentation within the criminal justice system. However, their overrepresentation in the justice system demands a coordinated, multisystem response that reduces or prevents justice involvement while addressing clinical, criminogenic, and substance use needs in a holistic manner.
To accomplish this goal, the community mental health system will have to develop and enhance existing cross-system collaborations with the substance use, criminal justice, and social service systems. Although we cannot expect that a community mental health system can solve the social problems of poverty or structural racism, we believe that if adequately supported, the community mental health system is in the best position to lead in the development of an integrated service system capable of addressing in a seamless manner the multiple treatment needs of justice-involved people with serious mental illness.